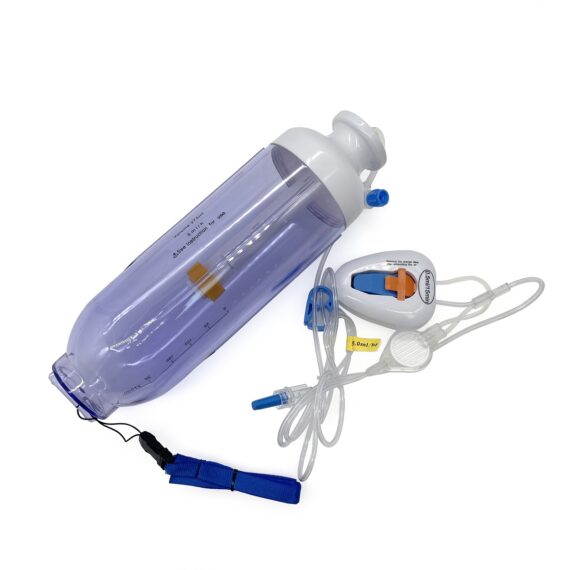
Elastomeric infusion pumps are medical devices used to slowly deliver medicines such as antibiotics, chemotherapy drugs, or painkillers into a patient’s body in a precise, controlled manner. These pumps offer portability and convenience over traditional intravenous methods, allowing patients greater freedom and improving their quality of life. This article will explore how elastomeric pumps work, common types available, benefits over other delivery methods, and important safety considerations for patients and caregivers.
How Elastomeric Pumps Work
All Elastomeric infusion pump operate on the simple principle of controlled elastic deformation. The pump utilizes a pre-filled reservoir made of flexible medical-grade rubber or silicone that is squeezed to deliver the drug content. Most models contain a one-way valve that prevents backflow and a regulated squeeze mechanism made of the elastic material. As the reservoir compresses and expands on a repeating cycle, it pushes out small, consistent amounts of fluid through tubing and into the patient. This gentle squeezing motion mimics a continuous intravenous infusion but can be worn discreetly and allows independent mobility. No electric power or batteries are needed.
Common Types of Elastomeric Pumps
There are a few different styles of elastomeric pumps on the market with variations in size, reservoir capacity, and features. One of the most basic and portable options is the balloon pump, which resembles a small inflatable balloon. Larger cylindrical designs with interchangeable reservoirs holding 50-150mL are also widely used. More advanced versions may have proprietary squeeze mechanisms, digital controls, and alarms to monitor delivery settings and alerts. Ambulatory pumps meant for extended outpatient use can deliver drugs over 24 hours or longer before needing to be refilled or replaced. Implantable pumps are sometimes used for chronic pain or spasticity treatment.
Benefits Over Intravenous Delivery
The primary advantages of elastomeric pumps compared to traditional intravenous infusion are convenience and mobility. Patients are not tethered to an IV pole or pump machine and can be ambulant rather than bedridden. This improves quality of life and allows for greater participation in normal daily activities. Elastomeric pumps are also more cost effective for administering long-term outpatient therapies versus frequent clinic or home health nurse visits. They eliminate the inconvenience of accessing peripheral IV sites which can become sore or infected if left in place for many days. For patients requiring lengthy infusions, elastomeric pumps provide a discreet, durable solution.
Safety Considerations
While Elastomeric infusion pumps aim to simplify drug delivery, there are some safety issues to keep in mind. Air bubbles in the tubing or disconnection from the catheter access point pose risks, so lines must be primed properly and secured. The squeeze mechanism can malfunction if damaged or worn down over time, leading to inaccurate dosing. Users and caregivers need proper training to fill, operate and maintain the device according to instructions. Signs of leaks, blockages or declining fluid levels should prompt inspection and potentially early replacement. Strict hygiene is also required when accessing the inlet and outlet ports. Overall, elastomeric pumps improve mobility but still warrant monitoring to ensure consistent, controlled infusion as intended by the treatment plan.
Choosing the Right Elastomeric Pump
When selecting an elastomeric pump, it is important to consider the clinical situation and individual patient factors. More urgent inpatient needs may warrant ambulatory pumps with shorter lifespans, while outpatient therapies demand pumps rated for multi-day use. Catheter type, planned infusion duration, medication attributes and prescribed flow rates all influence which design and reservoir capacity is best suited. Patient mobility, dexterity and visual or cognitive abilities also guide choosing lightweight, simple models versus more sophisticated digital devices. Consultation between the healthcare team, patient and device manufacturer ensures the optimal pump model is prescribed to safely and effectively deliver therapy as intended.
Advancements and Future Directions
Technology improvements continue to enhance elastomeric pump design. While the basic operating principle remains elastic deformation, features like precision tubing without external valves help standardize flow patterns. “Smart pumps” integrate sensors and programming to better regulate delivery and monitor for occlusion or empty reservoirs. Some connect via Bluetooth to smartphone apps for remote monitoring by caregivers. Implantable pumps are being miniaturized for localized delivery directly to targeted tissues like the spinal cord or brain. Regional anesthesia using elastomeric peripheral nerve blocks shows promise. Looking forward, 3D printing may enable patient-customized devices. Control through injectable hydrogels actuated by ultrasound could yield even more freedom and discretion. Overall, elastomeric pumps adapt well to evolving care needs through intelligent materials and connectivity innovations.
In summary, elastomeric infusion pumps provide a portable, ambulatory alternative to traditional intravenous deliverymethods. Their simple yet controlled mechanism allows consistent drug administration without tubing or machinery. Across inpatient and outpatient settings, elastomeric pumps improve quality of life by enabling mobility during long-term infusions. While safety considerations require attention, trained users benefit from discretion and freedom. Advancing materials and integration of sensors continue enhancing performance to precisely meet evolving therapy needs. Elastomeric pumps undoubtedly improve patient experience and outcomes through convenient drug delivery over extended periods.
*Note:
1. Source: Coherent Market Insights, Public sources, Desk research
2. We have leveraged AI tools to mine information and compile it