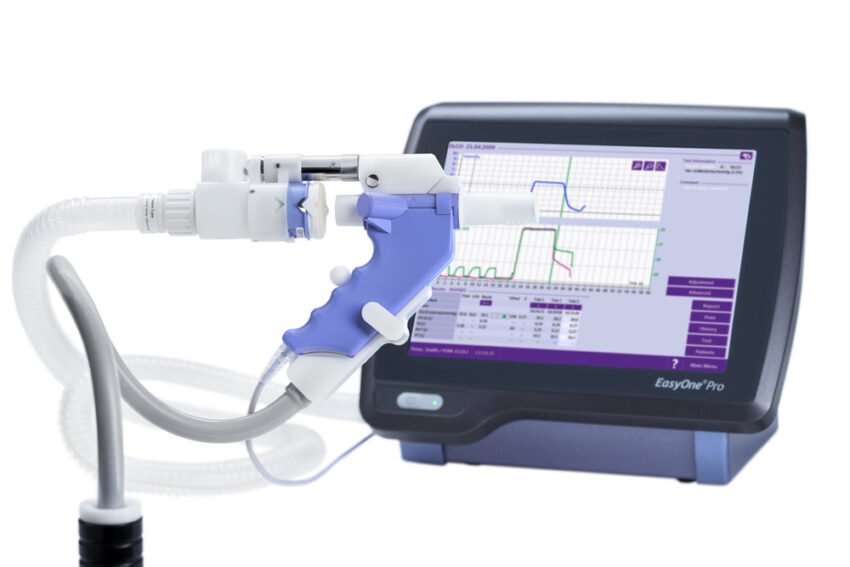
What is a Spirometer?
A spirometer is a simple medical device used to measure lung function, specifically the amount (volume) and/or speed (flow) of air that can be inhaled and exhaled. Spirometers are often used by doctors and respiratory therapists to test for and diagnose respiratory diseases such as asthma or Chronic Obstructive Pulmonary Disease (COPD).
The basic principle behind spirometry testing is that a person breathes through a mouthpiece or nozzle connected to the spirometer device. As the person inhales and exhales, the spirometer measures how much air enters and leaves the lungs and how quickly the air moves. Various lung function metrics like forced vital capacity (FVC), forced expiratory volume in 1 second (FEV1), FEV1/FVC ratio, peak expiratory flow rate (PEFR) and more can be evaluated.
How does a Spirometer work?
Most modern Spirometers use either the flow-sensing or the volume displacement principle to record breath flow rates and volumes.
In flow-sensing spirometers, air flow is measured directly using mechanisms like hot-wire anemometry. As exhaled or inhaled air flows through a small mesh/screen containing heated wires, it cools the wires slightly. The change in resistance is used to calculate flow rates.
Volume displacement spirometers work by having the patient breathe into or out of a chamber of known volume. The movement of the piston inside the chamber due to breathing displaces a known air volume. By measuring the displacement over time, flow and volume data can be derived.
Some advanced digital spirometers use integrated microprocessors and sensors to instantly analyze breath flow and volume waveforms on a backlit display screen in real-time. Test results are immediately available for clinical evaluation.
Uses of Spirometry Testing
Spirometry is commonly used to:
– Diagnose respiratory conditions: Reduced airflow measures on spirometry often indicate asthma, COPD, pneumonia, lung fibrosis or cystic fibrosis. It aids early detection.
– Monitor disease progression: Serial spirometry tests are helpful to track how a lung disease is progressing over time and respond to treatment changes accordingly.
– Assess treatment effectiveness: Spirometry before and after using bronchodilators helps determine if medications are successfully opening up airways. It guides management decisions.
– Screen for occupational lung diseases: Workers exposed to respiratory hazards undergo periodic spirometry to detect early signs of occupational lung conditions like silicosis, asbestosis, coal worker’s pneumoconiosis.
– Assess impact of surgery/injury: Lung function is evaluated pre and post surgery involving the chest or following severe chest trauma to monitor recovery.
– Family planning advise: Identifying reduced lung function in a family aids counseling on risks of passing lung disorders to offspring.
Spirometry is a important, noninvasive and relatively low-cost diagnostic tool widely used in pulmonary medicine.
Variations in Spirometry Devices
There are different types of spirometer devices suited for specific needs:
– Table-top Lab Spirometers: Sophisticated systems for clinical pulmonary function testing with plethysmography capability.
– Portable Spirometers: Handheld units ideal for point-of-care testing and field screenings due to their compact size and ease of use. Battery operated.
– Bedside Spirometers: Easy to maneuver devices meant for testing patients confined to beds or with limited mobility.
– Pediatric Spirometers: Small volume chambers and different air flow sensors adjusted for testing lung functions in infants and children.
– Waterless Spirometers: No water/volume displacement system required. Use principles like hot-wire anemometry directly.
– Specialized Spirometry Software: Advanced programs to support complex lung modeling, interpretive reports and data tracking over time. Integrate with EMR systems.
The choice depends on required functionality, budget, space availability and target patient population like adults, kids or those needing bedside testing.
Spirometry – Safety, Quality and Infection Control
Proper technique and hygienic practices during spirometry are essential to ensure accurate, reproducible results and prevent cross-contamination:
– Single-use mouthpieces or sterilizable, autoclavable mouthpieces reduce infection risks. Disposable filters are another option.
– Patients should not have eaten, smoked, exercised or used respiratory medications for a period prior to the test as per guidelines.
– Nose clips help make a tight mouth seal. Multiple efforts with best trial documented is recommended.
– Spirometers must be calibrated regularly using 3-liter syringes or rotameters per manufactures guidelines and quality control standards.
– Routine disinfection and maintenance is important. Filters and water/solution in wet spirometers needs periodic changing for safety.
– Staff training and competency assessment in spirometry testing technique is vital to minimizing errors and improper performance affecting results.
Adhering to these protocols ensures spirometry analysis provides reliable, accurate readings that aid appropriate clinical decision making. It also protects both patients and health workers.
Simple and highly useful, spirometry has emerged as a cornerstone of evaluating lung health conditions. When performed correctly by trained individuals, it offers invaluable insights supporting diagnosis, monitoring disease progression/improvement and guiding management of respiratory illnesses. Regular quality checks and adherence to infection control best practices with this diagnostic procedure also helps deliver safe patient care. Spirometry thus remains a mainstay respiratory diagnostic test worldwide.
*Note:
1. Source: Coherent Market Insights, Public sources, Desk research
2. We have leveraged AI tools to mine information and compile it